|
The purpose of this retrospective study was to assess post-ACLR differences in International Knee Documentation Committee Subjective Knee Form (IKDC) scores in patients who did not (NB) and did (FB) receive perioperative FNB. Purpose: Femoral nerve blocks (FNB) for anterior cruciate ligament reconstruction (ACLR) can effectively reduce post-operative pain, though this is tempered with the potential for quadriceps weakness, and subsequent concerns regarding impeded rehabilitation. The medial cord is the origin of the median nerve and contributes to the ulnar. The lateral cord is the origin of the musculocutaneous nerve, which together with the medial cord contributes to the median nerve. From the cords, individual nerves form as they branch and descend to the distal end of the extremity. 6 The nerve trunks divide and interconnect to form the lateral, medial, and posterior cords. The brachial plexus innervates the shoulder and arm. The brachial nerve plexus is made up of nerves originating from the lower four cervical and the first tho- racic spinal nerves (ie, C 5 -T 1 ). To understand PNBs of the upper extremities, it is important to understand the anatomy of the brachial nerve plexus ( Figure 1). The femoral and sciatic blocks involve blocking nerves that arise from the lumbar and lumbosacral plexus and are used for surgeries of the lower extremities. The first three involve blockade of the brachial nerve plexus and are used for surgeries of the upper extremities. Common locations for the administration of outpatient PNBs are the interscalene, supraclavicular, and axillary plexus and the femoral and sciatic nerves. Consequently, a surgeon is able to perform surgery on an extremity that has been “blocked” without using general anesthesia, and the patient usually requires fewer postoperative narcotics for pain. Depending on where and how the anesthetic agent is injected, sensory, motor, and/or sympathetic pathways are affected, and the patient loses his or her ability to move or feel the blocked extremity. For a PNB, the anesthesia professional injects the local anesthesia near or around a nerve or nerve plexus that supplies an entire region (eg, a plexus innervating an extremity), which affects the sensory and motor capability of the nerves that carry impulses to the extremity. When local anesthesia is injected into an area of surface skin, the nerve endings at the skin are anesthetized. 5 This disruption in sodium exchange interferes with nerve impulse pathways between the anesthetized area and the brain. 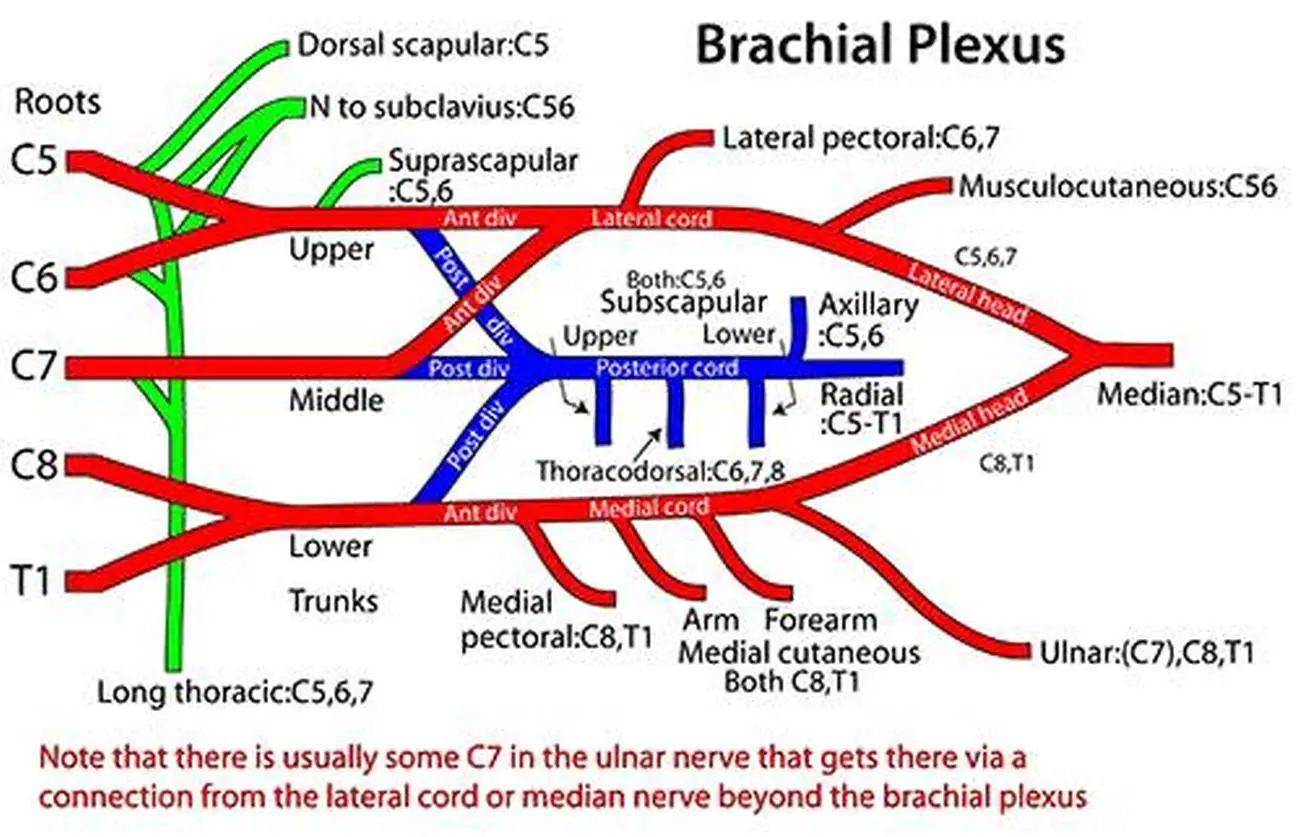
5 Local anesthesia prevents pain by interfering with the nerve membrane’s permeability to sodium. 5 Local anesthesia provides a reversible regional loss of sensation that reduces pain and facilitates the performance of surgical procedures without many of the risks of general anesthesia. 4 Today, physicians have a wide variety of methods available for local anesthesia administration. 4 Fewer negative respiratory effects (eg, respiratory depression) and cardiovascular effects (eg, tachyarrhythmias, seizures) compared with general anesthesia and the stability of local analgesia have increased its popularity. During the past 150 years, many types of local anesthesia have been extensively re- searched and developed. 4 In 1860, cocaine was first used as a local anesthesia. In 1845, Dr Rynd described the idea of applying a solution of morphine around a peripheral nerve to relieve neuralgic pain. 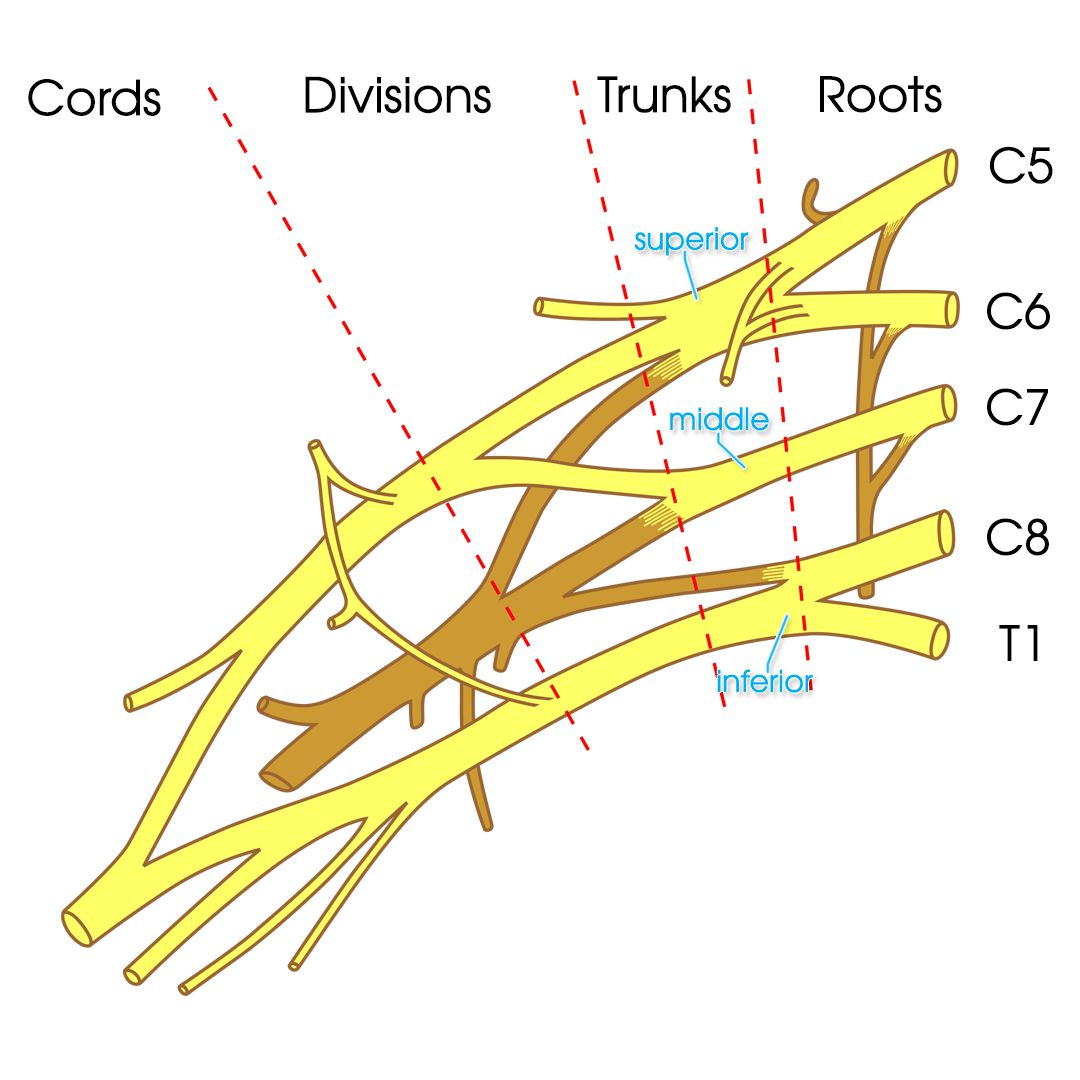
3 The invention of the syringe and needle was a significant step in the evolution of local anesthesia. Francis Rynd, a physician in Ireland, invented the hypodermic syringe in 1844 and administered the world’s first subcutaneous injection.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
